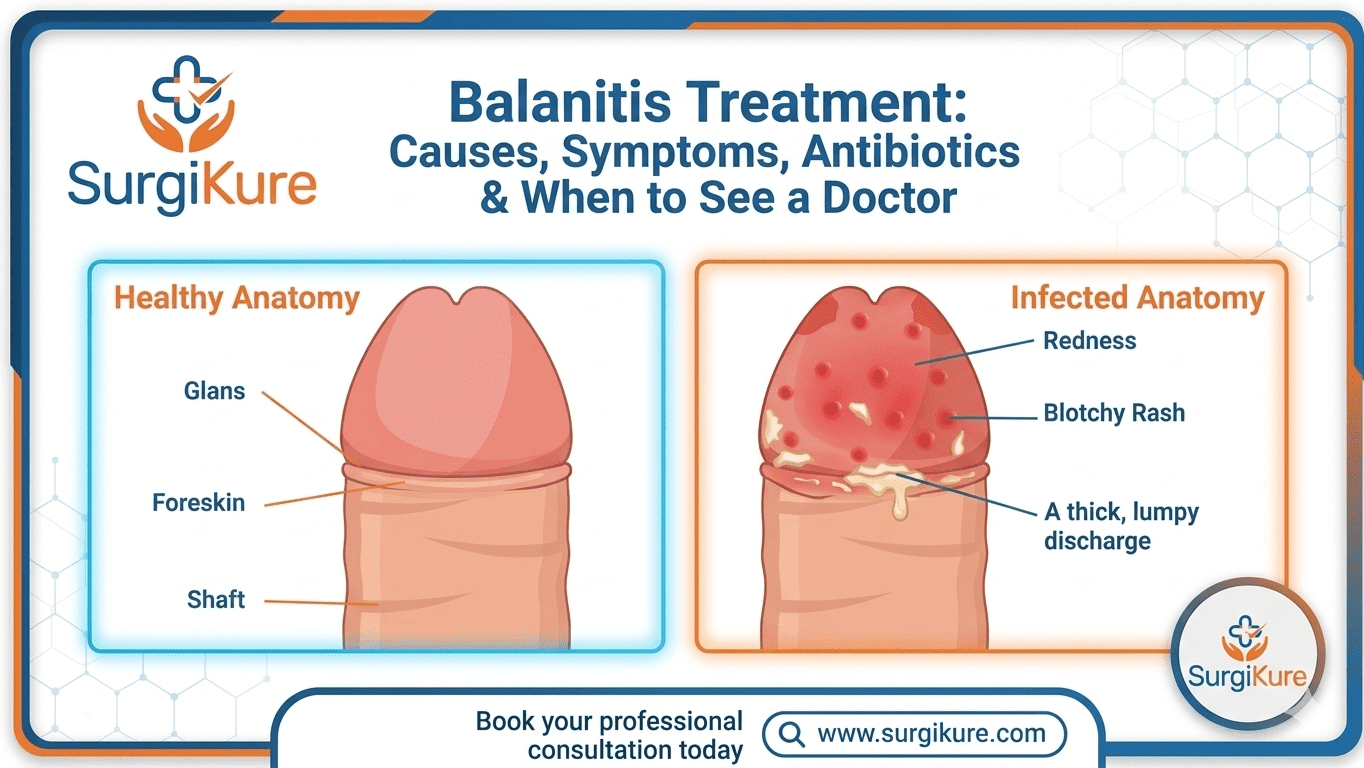
Balanitis Treatment: Causes, Symptoms, Antibiotics & When to See a Doctor
If you’ve noticed redness, itching, or discomfort on the head of your penis, you might be dealing with balanitis—and you’re definitely not alone. This common condition affects men of all ages, yet many feel too embarrassed to seek help. The good news? Balanitis is highly treatable, and understanding what causes it is the first step toward relief.
In this comprehensive guide, we’ll walk you through everything you need to know about balanitis treatments, from home remedies to medical interventions, and help you determine when it’s time to see a doctor.
What Is Balanitis? Understanding the Condition
Balanitis is inflammation of the glans (the head of the penis). The term comes from the Greek word “balanos,” meaning acorn, which describes the shape of the glans. When inflammation extends to include the foreskin as well, the condition is called balanoposthitis—a closely related condition that shares many similarities with balanitis.
Understanding the difference between balanitis vs balanoposthitis is important for treatment purposes. While balanitis affects only the glans, balanoposthitis involves both the glans and the prepuce (foreskin). Both conditions cause similar symptoms and often require similar treatment approaches.
The condition is characterized by swelling, redness, and irritation that can range from mild discomfort to severe pain, making daily activities and urination uncomfortable.

Common Causes of Balanitis
Balanitis causes are varied and often interconnected. Identifying the underlying cause is crucial for effective balanitis treatment:
Fungal Infections
The most common cause of balanitis is a yeast infection caused by Candida albicans. Men with diabetes or weakened immune systems are particularly susceptible. Poor hygiene or moisture trapped under the foreskin creates an ideal environment for fungal growth.
Bacterial Infections
Various bacteria, including Staphylococcus and Streptococcus, can cause balanitis. These infections often develop following sexual contact or from poor hygiene practices.
Poor Hygiene
Inadequate cleaning, especially in uncircumcised men, allows sweat, urine, and dead skin cells to accumulate beneath the foreskin, creating an environment where infection thrives.
Sexual Transmission
Balanitis can develop after sexual contact with a partner who has a vaginal yeast infection or other sexually transmitted infections.
Irritant Dermatitis
Harsh soaps, detergents, latex condoms, or spermicides can irritate the sensitive skin of the glans, causing inflammation and redness.
Phimosis
When the foreskin is too tight to retract, it creates a moist environment that promotes bacterial and fungal growth.
Diabetes
High blood sugar levels increase glucose in urine, which feeds candida and other organisms, making diabetic men more prone to balanitis.
Other Contributing Factors
Poor sexual hygiene, moisture from sweat or urine, antibiotic use, and weakened immunity can all contribute to balanitis development.
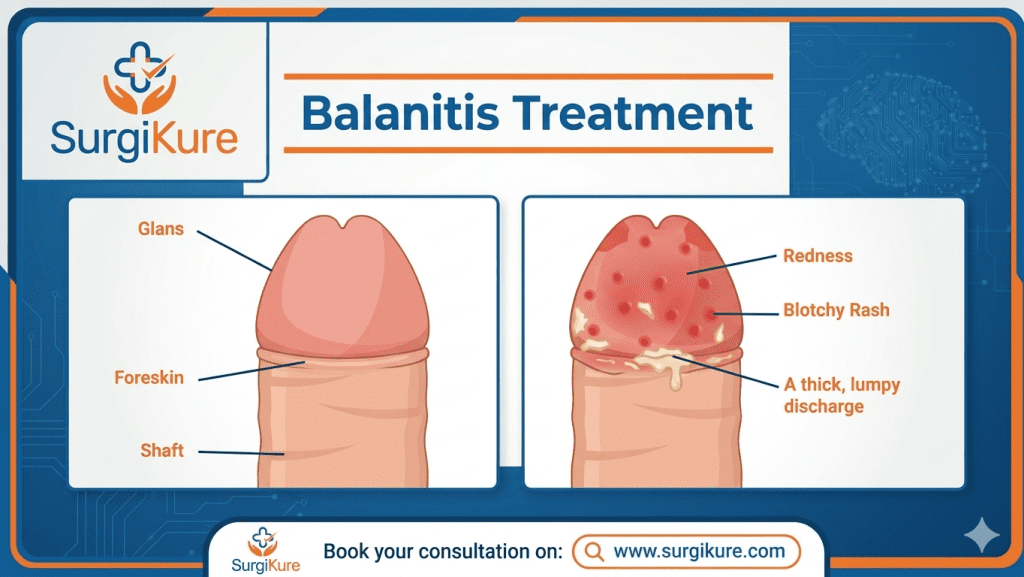
Recognizing Balanitis Symptoms
Balanitis symptoms can develop gradually or appear suddenly. Early recognition helps you seek timely treatment. Common signs include:
- Redness and swelling of the glans
- Itching and burning sensation, particularly during urination
- Discharge that may be yellowish or clear
- Unpleasant odor from the affected area
- Pain during sexual intercourse or masturbation
- Difficulty retracting the foreskin (in balanoposthitis cases)
- Skin changes including cracks, peeling, or unusual texture
- Pustules or spots on the glans surface
If you notice any combination of these symptoms, it’s important not to ignore them. While balanitis is rarely serious, untreated cases can lead to complications like phimosis or paraphimosis.


Balanitis Treatment Options
The approach to balanitis treatment depends on the underlying cause. Here’s what you can expect:
Antifungal Treatments
For fungal balanitis (the most common type), antifungal creams are the first-line treatment:
- Topical creams: Clotrimazole, miconazole, and terbinafine are applied directly to the affected area
- Duration: Usually 7-14 days of twice-daily application
- Effectiveness: Most fungal infections clear within this timeframe
If topical treatments don’t work, oral antifungal medications like fluconazole may be prescribed.
Antibiotics for Bacterial Balanitis
When bacterial infection is the culprit, balanoposthitis antibiotics or specific balanitis antibiotics are necessary:
- Topical antibiotics: Mupirocin or neomycin ointments for mild to moderate cases
- Oral antibiotics: For more severe infections or systemic involvement
- Common choices: Amoxicillin, cephalexin, or fluoroquinolones depending on bacterial sensitivity
The choice of antibiotic depends on bacterial culture results when available, ensuring targeted and effective treatment.
Corticosteroid Creams
For irritant or allergic balanitis, mild topical corticosteroids (like hydrocortisone 1%) can reduce inflammation. These are typically not used alone but combined with antifungal or antibiotic treatments.
Oral Medications
In some cases, particularly with severe infections or systemic involvement, oral medications may be necessary alongside topical treatments.
Advanced Laser Treatment
For recurrent or resistant cases, laser therapy has emerged as an effective option. At SurgiKure, we offer advanced laser treatment for persistent balanitis that doesn’t respond to conventional therapies. Laser treatment works by:
- Reducing bacterial and fungal load through precise thermal effects
- Promoting tissue healing and regeneration
- Minimizing scarring and complications
- Providing long-term relief for chronic cases
Balanitis Home Remedy and Self-Care Measures
While professional treatment is essential, these home remedies can complement medical care and speed recovery:
Keep the Area Clean and Dry
- Gently wash the glans with warm water twice daily
- Use mild, fragrance-free soap to avoid irritation
- Pat dry thoroughly with a soft towel
- Avoid moisture buildup under the foreskin
Avoid Irritants
- Stop using scented soaps, body washes, or detergents
- Switch to hypoallergenic alternatives
- Avoid latex condoms if you have latex sensitivity
- Wear breathable cotton underwear
Saltwater Soaks
- Soak the affected area in warm saltwater (1 teaspoon salt in 1 cup water) for 5-10 minutes
- This natural balanitis home remedy can reduce inflammation and prevent secondary infection
- Repeat 2-3 times daily for relief
Pain Management
- Over-the-counter pain relievers like ibuprofen can help manage discomfort
- Avoid sexual activity until symptoms resolve
Lifestyle Changes
- Maintain good blood sugar control if diabetic
- Avoid excessive moisture and sweating in the area
- Wear loose-fitting clothing
- Ensure proper hygiene during and after sexual activity
Balanitis vs Balanoposthitis: Key Differences
While these conditions are similar and often coexist, understanding the distinction helps guide treatment:
| Feature | Balanitis | Balanoposthitis |
|—|—|—|
| Affected Area | Glans only | Glans and foreskin |
| Symptom Severity | Generally mild to moderate | Often more pronounced |
| Foreskin Involvement | Minimal or none | Significant involvement |
| Complication Risk | Lower | Higher (phimosis/paraphimosis) |
| Treatment | Topical medications usually sufficient | May require stronger interventions |
Both conditions respond well to proper treatment when addressed early. However, balanoposthitis may require circumcision if phimosis develops.
When to See a Doctor: Warning Signs You Shouldn’t Ignore
While many cases of balanitis resolve with home care and over-the-counter treatments, certain situations warrant professional medical attention:
Seek Medical Help If:
- Symptoms persist beyond 2 weeks despite home treatment
- Symptoms worsen or spread to other areas
- You develop fever, chills, or systemic symptoms
- Discharge becomes thick, foul-smelling, or bloody
- You experience severe pain or inability to urinate
- The condition recurs frequently (more than 4 times yearly)
- You have diabetes or a weakened immune system
- Sexual contact has exposed you to potential infection
- You notice signs of phimosis or paraphimosis (inability to retract or reduce foreskin)
- Home remedies and over-the-counter treatments fail
Don’t let embarrassment delay seeking care. Balanitis is a medical condition like any other, and timely treatment prevents complications and discomfort.

Why Choose SurgiKure for Balanitis Treatment in Hyderabad, Visakhapatnam & Vijayawada
At SurgiKure, we understand that discussing intimate health concerns can feel uncomfortable. That’s why we’ve built a practice centered on patient dignity, expert care, and cutting-edge treatment options.
Our Advantages:
- Specialized Expertise: Our surgeons have extensive experience treating all types of balanitis and related genital conditions
- Comprehensive Diagnosis: We use advanced diagnostic techniques to identify the exact cause of your balanitis
- Multiple Treatment Options: From topical medications to advanced laser therapy, we offer solutions tailored to your specific condition
- Discreet and Compassionate Care: We maintain strict confidentiality and create a judgment-free environment
- Advanced Technology: Our clinics in Hyderabad, Visakhapatnam, and Vijayawada are equipped with state-of-the-art diagnostic and treatment equipment
- Proven Results: We’ve successfully treated hundreds of balanitis cases with excellent outcomes
Clinical Documentation: During your consultation, our doctors can show you real clinical images and case studies demonstrating successful balanitis treatment outcomes.
Prevention: The Best Medicine
Once you’ve experienced balanitis, preventing recurrence becomes a priority:
- Maintain excellent genital hygiene: Wash daily with warm water and mild soap
- Keep dry: Change out of wet clothes promptly, especially after swimming or exercise
- Use protection wisely: Use condoms consistently and ensure your partner is infection-free
- Manage diabetes: Tight blood sugar control significantly reduces balanitis risk
- Consider circumcision: If you have recurrent balanitis with phimosis, circumcision can be curative
- Regular check-ups: Annual genital health check-ups can catch early signs of problems
Key Takeaways
- Balanitis is inflammation of the glans, most commonly caused by fungal infections, particularly Candida albicans
- Multiple balanitis causes exist, including bacterial infections, poor hygiene, diabetes, and irritants
- Balanitis treatments range from topical antifungal creams to oral antibiotics, depending on the underlying cause
- Home remedies like saltwater soaks and proper hygiene can complement professional treatment
- Balanoposthitis involves both the glans and foreskin, requiring similar but sometimes more intensive treatment
- Laser treatment offers advanced options for recurrent or resistant cases
- Prevention through hygiene and lifestyle changes is highly effective
- See a doctor if symptoms persist beyond 2 weeks or if you notice warning signs
Frequently Asked Questions (FAQ)
Q: Can balanitis go away on its own?
A: Mild cases might improve with improved hygiene, but most require medical treatment. Untreated balanitis often worsens and can lead to complications.
Q: How long does balanitis treatment take?
A: Most cases resolve within 7-14 days with proper topical treatment. Severe or complicated cases may take longer.
Q: Is balanitis contagious?
A: Yes, if caused by infection. You can transmit it to sexual partners. Avoid sexual contact during treatment.
Q: Can circumcision prevent balanitis?
A: Yes, circumcision significantly reduces the risk, especially for men with recurrent balanitis and phimosis.
Q: What’s the cure of balanitis?
A: The cure depends on the cause—antifungal creams for fungal cases, antibiotics for bacterial infections, and lifestyle changes for irritant-based balanitis. Laser treatment is effective for resistant cases.
Q: Should I use balanoposthitis antibiotics for regular balanitis?
A: Only if bacterial infection is confirmed. Fungal balanitis requires antifungals, not antibiotics.
Your Path to Relief Starts Here
Balanitis doesn’t have to be a source of ongoing discomfort or embarrassment. With proper diagnosis and the right balanitis treatment, you can achieve relief and return to normal life.
At SurgiKure, we’re ready to help. Our experienced team across Hyderabad, Visakhapatnam, and Vijayawada specializes in treating all types of genital conditions with the latest medical advances, including laser treatment options.
Book Your Free Consultation Today and discuss your symptoms with a specialized surgeon who understands your concerns. During your consultation, we can review real clinical images, discuss your specific condition, and create a personalized treatment plan that works for you.
Don’t let balanitis symptoms persist—reach out to SurgiKure and take the first step toward relief. Your health and comfort matter, and we’re here to help.
[Schedule Your Free Consultation Now → Please contact our health care experts for details: 7670968977 (Hyderabad), 7797377779 (Vizag/Vijayawada)]