The surgical landscape of male circumcision has undergone a radical transformation with the introduction of automated, minimally invasive technologies. Stapler circumcision, primarily utilizing the ZSR stapler device or circumcision anastomat, has emerged as a preferred clinical alternative to traditional scalpel-based methods due to its precision, standardized results, and accelerated healing profile. This report provides an exhaustive examination of the physiological, clinical, and aesthetic aspects of the procedure, with a specific focus on the visual milestones captured through stapler circumcision recovery photos across the healing spectrum.
Historical and Technological Evolution of Circumcision
The practice of circumcision, one of the oldest surgical procedures known to humanity, has transitioned from ritualistic origins to a highly regulated medical intervention. Traditionally, methods such as the dorsal slit, forceps-guided procedure, and sleeve resection were the standard recommendations of the World Health Organization (WHO). While effective, these conventional techniques are often associated with variable operative times, significant intraoperative bleeding, and a dependency on the individual surgeon’s suturing skills.
The advent of the stapler device, particularly the ZSR technology, represents a mechanical leap in surgical standardization. The device integrates the cutting and sealing phases into a single motion, utilizing a circular surgical blade and a ring of titanium staples. This automation minimizes manual handling of tissue, thereby reducing the risk of tissue trauma and subsequent inflammatory responses.
Comparative Overview of Surgical Parameters
The following table highlights the clinical differences between the stapler method and conventional surgical approaches, providing a quantitative basis for the shift toward automated technology.
| Feature | Stapler Circumcision (ZSR) | Traditional Scalpel Circumcision |
| Typical Procedure Duration | 5–15 minutes | 30–60 minutes |
| Hemostasis Mechanism | Mechanical compression staples | Manual ligatures or electrocautery |
| Wound Closure | Titanium staples and silicone ring | Absorbable or non-absorbable sutures |
| Intraoperative Blood Loss | Minimal ($<10$ mL) | Moderate ($15$–$40$ mL) |
| Post-Operative Pain (VAS Score) | Significantly lower (3.2 on Day 1) | Higher (5.1 on Day 1) |
| Surgical Skill Dependency | Low (Standardized by device) | High (Dependent on suturing technique) |
Anatomical Considerations and Medical Indications
A thorough understanding of the penile anatomy is essential for both the surgeon performing the procedure and the patient monitoring their recovery. The prepuce, or foreskin, is a specialized, multi-layered structure consisting of the outer skin (keratinized squamous epithelium), a middle layer of dartos muscle and loose connective tissue, and an inner mucosal layer. This tissue provides protective coverage for the glans penis and contains a high density of sensory nerve endings.
Circumcision is indicated for a variety of medical conditions that compromise urological health or sexual function. Phimosis remains the leading indication, characterized by a foreskin that is too tight to be retracted over the glans, often leading to pain during erections and difficulty maintaining hygiene. Paraphimosis, a more acute condition where the foreskin becomes trapped behind the glans, constitutes a medical emergency requiring immediate intervention to prevent vascular necrosis.
Pathological Indications for Circumcision
- Balanitis and Posthitis: Chronic or recurrent inflammation of the glans and prepuce, frequently exacerbated by diabetes mellitus.
- Recurrent Urinary Tract Infections (UTIs): The prepuce can serve as a reservoir for bacterial pathogens, increasing the risk of ascending infections.
- Penile Malignancies: Circumcision is associated with a reduced risk of penile cancer and localized carcinoma.
- Lichen Sclerosus: A scarring condition that can lead to severe phimosis and urinary obstruction.
The Stapler Circumcision Procedure: A Clinical Walkthrough
The ZSR stapler procedure is typically performed as an outpatient or “day case” surgery under local anesthesia. The preparatory phase involves thorough disinfection and the administration of a dorsal penile nerve block or a ring block using anesthetic agents such as lidocaine or bupivacaine.
Once the area is desensitized, the surgeon measures the diameter of the glans to select the appropriate device size. The foreskin is retracted, and a safety bell or rod is positioned over the glans for protection. The stapler is then aligned over the bell, and the trigger is activated. This single motion performs three simultaneous functions: it excises the redundant foreskin, applies a circular row of titanium staples to the wound edges, and secures a silicone ring that aids in hemostasis and protects the incision.
Visual Progression: Stapler Circumcision Recovery Photos
The visual changes following stapler circumcision follow a predictable physiological sequence. Understanding these milestones through a clinical lens allows for better patient self-monitoring and early detection of rare complications.
Photos Before Circumcision & After 1 Day
Prior to surgery, the patient’s anatomy may demonstrate the pathological characteristics that necessitated the procedure, such as the white, fibrotic ring of phimosis or the erythematous, swollen appearance of chronic balanoposthitis. The glans is often completely covered and may be sensitive to even minor manipulation.
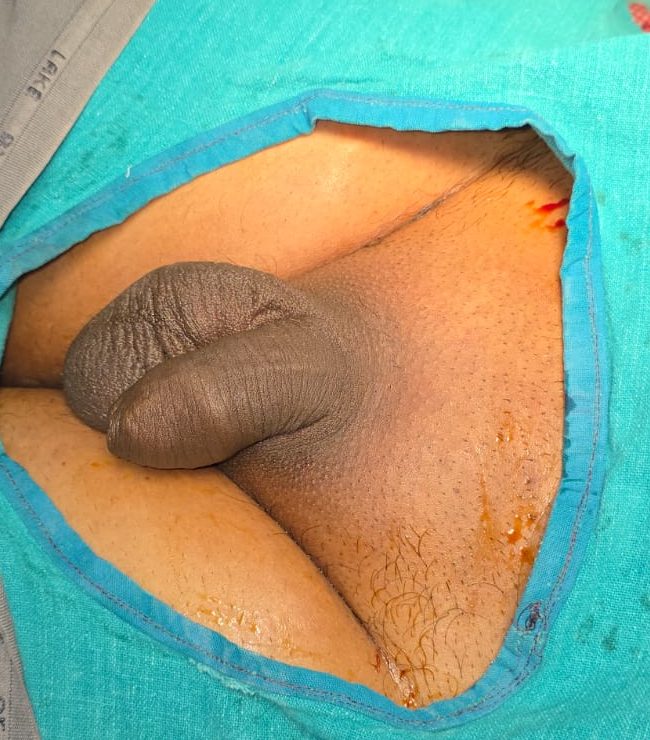

In the first 24 hours post-operation, the surgical site is in the acute inflammatory phase. The glans, now fully exposed for the first time in many patients, will appear glossy, red, and potentially edematous. A tight compression dressing is usually in place to manage initial swelling and prevent minor oozing.
Clinical Observations at Day 1:
- Glans Hypersensitivity: The newly exposed mucosa is highly reactive to contact with clothing or bandages.
- Edema: Swelling is most pronounced just behind the glans, where the lymphatic drainage has been temporarily disrupted.
- Bruising: Subcutaneous ecchymosis (bruising) is common around the base of the penis and the incision site.


Photos After 1 Week
By day seven, the patient has entered the proliferative phase of wound healing. The initial intense inflammation has begun to subside, and the body starts the process of epithelialization.
Clinical Observations at 1 Week:
- Yellowish Film: It is normal to observe a yellowish or off-white film on the glans or near the incision. This is fibrin—a protein involved in blood clotting and tissue repair—and should not be mistaken for pus.
- Scab Formation: Small scabs may form around the staples.
- Device Status: The silicone ring and titanium staples are still firmly attached to the wound line.


Photos After 2 Weeks
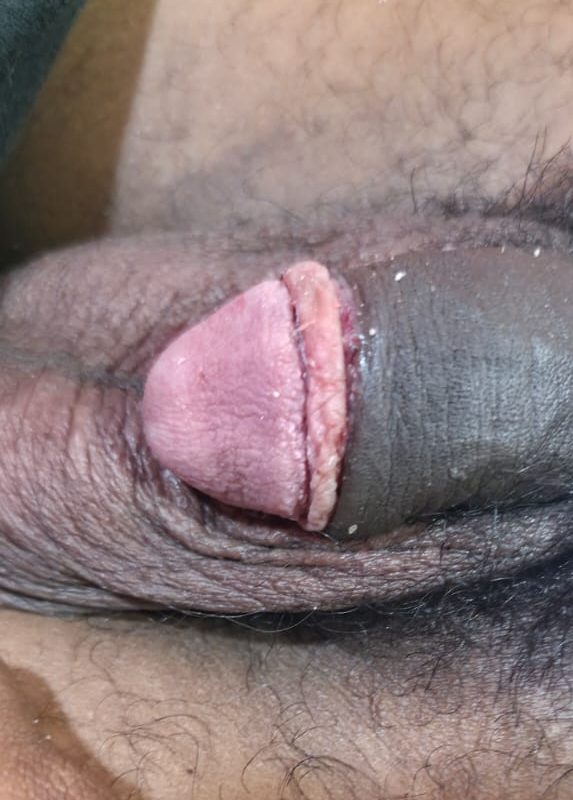
The second week is characterized by the remodeling of the tissue and the mechanical detachment of the stapler hardware. For most adults, the silicone ring and staples shed naturally between days 10 and 14.
Clinical Observations at 2 Weeks:
- Hardware Detachment: The staples begin to loosen and fall off as the underlying skin heals.
- Incision Appearance: The resulting scar line is remarkably uniform and linear, lacking the “cross-hatch” marks often seen with traditional sutures.
- Sensitivity Reduction: The glans begins to develop a dryer, less sensitive epithelial layer.

Physiological Management of the Recovery Phase
The success of stapler circumcision depends heavily on the management of post-operative symptoms, particularly pain, swelling, and the involuntary expansion of penile tissue.
Pain Management Protocols
Post-operative pain following the stapler method is generally reported as mild to moderate. Discomfort typically peaks within the first 3 to 5 days.
| Medication Type | Clinical Application | Dosage/Instructions |
| Acetaminophen (Tylenol) | Mild to moderate baseline pain | Follow packaging directions; avoid combining with other paracetamol products |
| NSAIDs (Ibuprofen) | Managing inflammation and swelling | Take with food to prevent gastric irritation |
| Opioids (Vicodin/Codeine) | Severe breakthroughs (rare for ZSR) | Use only as prescribed; avoid driving or operating machinery |
| Topical Anesthetics | Managing glans hypersensitivity | Apply lignocaine jelly or petroleum jelly to the glans to reduce friction |
Management of Nocturnal and Morning Erections
One of the unique challenges in adult circumcision recovery is the occurrence of involuntary erections during sleep. These erections put significant mechanical stress on the healing incision and the staples.
Tactical Recommendations for Erection Control:
- Bladder Management: Emptying the bladder before sleep and waking up once during the night to urinate can reduce the physiological triggers for nocturnal erections.
- Temperature Shock: If an erection occurs, standing on a cold floor with bare feet can help redirect blood flow and reduce penile turgidity.
- Positioning: Sleeping in a side-lying position with knees bent (fetal position) may alleviate tension on the surgical site.
- Ice Application: Applying a wrapped ice pack to the groin area or the base of the penis for 5–10 minutes can provide rapid cooling and numbing.
Wound Care and Hygiene Standards
Proper hygiene is the primary defense against post-operative infection. The wound care regimen changes as the patient progresses through the recovery timeline.
Immediate Post-Op Care (0–48 Hours)
The initial compression dressing must remain in place for the first 24 to 48 hours to ensure hemostasis and protect the wound from environmental contaminants. If the bandage becomes soaked with urine or significantly soiled, it should be changed early after consultation with the care team.
Transition to Active Hygiene (48 Hours – 1 Week)
Once the initial dressing is removed, the patient can begin gentle cleaning. It is recommended to let warm water run over the incision rather than scrubbing the area. Patting the area dry with a clean towel or using a hair dryer on a cool setting is preferable to vigorous rubbing.
The application of petroleum jelly (Vaseline) or antibiotic ointment (Bacitracin) is advised to prevent the incision edges or the glans from sticking to underwear. This also helps keep the tissue supple as the staples begin to loosen.
Lifestyle and Activity Restrictions
| Activity | Restriction Period | Rationale |
| Bathing/Swimming | 4 weeks | Prolonged immersion increases infection risk and can prematurely soften staples |
| Strenuous Exercise | 2–4 weeks | High-impact activity can cause wound dehiscence or secondary bleeding |
| Sexual Activity | 4–6 weeks | Genital stimulation and friction can reopen the wound or displace the silicone ring |
| Return to Work | 2–3 days (office work) | Minimal downtime required for non-physically demanding roles |
Complications, Red Flags, and Clinical Intervention
While the complication rate for stapler circumcision is notably low (less than $2\%$ for major issues), patients must be vigilant in monitoring their recovery.
Distinguishing Between Normal Healing and Infection
A common concern among patients is the presence of discharge. It is vital to differentiate between the normal physiological response and a pathological infection.
- Normal Signs: Yellowish film (fibrin), mild redness, clear or slightly yellow fluid, and minor spotting.
- Infection Indicators (Red Flags): Foul-smelling discharge, thick green or white pus, spreading redness that feels hot to the touch, and a fever exceeding $38^{\circ}\text{C}$ ($100.4^{\circ}\text{F}$).
Managing Hardware Issues
The staples and silicone ring are designed to shed spontaneously. However, in approximately $12\%$ of cases, some staples may remain attached beyond the 3-week mark. If staples have not detached by day 21, the patient should visit their urologist for professional removal to prevent them from becoming embedded in the skin or causing excessive scarring.
Wound Dehiscence
Wound dehiscence—the partial or complete separation of the wound edges—is a rare complication ($<1\%$). This can occur due to premature strenuous activity or severe nocturnal erections that overpower the staples. If the wound edges appear to be separating, immediate medical attention is required. Small gaps may be managed with medical glue, while larger separations might require secondary suturing.
Long-term Aesthetic Results and Patient Satisfaction
One of the primary drivers for the adoption of stapler circumcision is the superior cosmetic outcome. Clinical studies have consistently shown that the ZSR method produces a neater, more symmetrical scar than traditional methods.
Evaluation of Cosmetic Outcomes
| Scale/Metric | Stapler Group Findings | Conventional Group Findings |
| POSAS Score | 9.1 (Higher satisfaction) | 7.5 (Lower satisfaction) |
| Stony Brook Scar Scale | Superior outcomes in texture and color | Variable results based on suture tension |
| Scar Hypertrophy Rate | Lower incidence with proper aftercare | Higher risk of “track marks” from sutures |
| Patient Satisfaction (%) | 76.7% rate results as “excellent” | 46.7% rate results as “excellent” |
The uniformity of the mechanical cut ensures that the edges align perfectly, promoting primary intention healing. This minimizes the formation of bulky scar tissue. For patients concerned with the “penile look,” the stapler method provides a result that is often indistinguishable from a natural, non-surgical appearance after full remodeling (typically 6 months post-op).
Pediatric Considerations in Stapler Circumcision
While the procedure is highly effective for adults, it is also widely utilized in pediatric urology. Children and infants exhibit different healing characteristics that necessitate specific care adjustments.
Healing Timelines by Age Group
- Infants (0–12 months): Rapid skin regeneration allows for complete healing within 7 to 10 days. Staples often fall off between days 5 and 7.
- Older Children (1–12 years): Healing takes slightly longer, generally 10 to 14 days. General anesthesia is often preferred for this age group to ensure patient comfort.
- Adolescents and Adults: Full structural healing takes 3 to 6 weeks, with a higher focus on managing nocturnal erections.
In infants, care must be taken with diaper management. Diapers should be fastened loosely to avoid pressure on the incision, and frequent changes are necessary to keep the area dry and free from irritants.
Economic Analysis: Cost vs. Benefit
The economic profile of stapler circumcision reflects its status as a premium, technology-driven procedure. While the upfront costs are higher than traditional surgery, the indirect savings associated with reduced operative time and faster return to work are significant.
Global Cost Comparison (Estimated)
| Region | Procedure Cost | Insurance/Claimability |
| Singapore | $1,888 – $3,000 SGD | Claimable under Medisave/Integrated Shields |
| India (Urban centers) | ₹25,000 – ₹45,000 INR | Variable; may require specific medical coding for coverage |
| United Kingdom | £1,500 – £2,500 GBP | Typically private pay; limited NHS availability for ZSR |
The disposable nature of the ZSR device adds to the procedural cost, but patients often justify the expense through the lens of improved comfort and aesthetic certainty.
Conclusion: The New Standard in Male Urological Care
Stapler circumcision has successfully transitioned from a novel surgical innovation to a cornerstone of modern male urological practice. By replacing the manual variability of scalpels and sutures with the mechanical precision of a specialized stapling device, the procedure offers a recovery experience that is faster, less painful, and cosmetically superior.
The visual milestones of recovery, as documented in stapler circumcision recovery photos, reveal a predictable trajectory of healing that transitions from acute inflammation to full tissue remodeling within a matter of weeks. While the technology provides the framework for success, the ultimate outcome remains a partnership between surgical precision and meticulous patient aftercare. For the modern male seeking a surgical solution for phimosis or other preputial conditions, the stapler method represents the optimal balance of efficiency, safety, and aesthetic satisfaction.
As clinical data continues to accumulate, it is likely that automated circumcision will continue to displace conventional techniques, setting a higher bar for what patients can expect from a routine surgical intervention. The integration of advanced wound-healing agents and refined device ergonomics will further solidify the role of the stapler as the gold standard in male circumcision.